Health and Society Assessment 3
Health issue代写 Discuss two different reasons for inequity between Indigenous Australians and non-Indigenous Australians in relation to this health issue.
| Extended ResponseTemplate |
Choose one health issue from the list below:
- Smoking
- Coronary heart disease
Answer all of the three questions below based on this one health issue.
Each extended response should be approximately 500 words in length each.
The reference list for all three extended response should be provided under the references heading of this template.
Question 1 Health issue代写Discuss two different reasons for inequity between Indigenous Australians and non-Indigenous Australians in relation to this health issue.
|
IntroductionTobacco use increases the risk of many diseases including cardiovascular disease, cancer, respiratory diseases, peripheral vascular disease and many others. This has resulted in high mortality and morbidity rates to the Australians (Marley et al, 2014; Pircher et al, 2012). In Australia, smoking has been contributed up to two-thirds of deaths on the average age of 10 years earlier than the non-smokers. Abstaining from smoking reduces mortality (Banks et al, 2015). Tobacco use has greatly contributed to the disease burden in indigenous Australian (12% of the total burden) and has created 23% health gap between indigenous and non-indigenous Australia in 2011 (AIHW, 2016f) The 2014-15 Social Survey have the most recent data on indigenous smoking rates. From the survey, 42% of the indigenous Australians aged 15 years and over, were the current smokers. According to the survey, there is 2.7 times prevalence of smoking higher in indigenous Australians than non-indigenous Australians. Reasons for inequalities Socioeconomic problems and education inequity Health issue代写Health behaviors and risk factors are found in the complexity of socioeconomic, family and community factors. “Inequities in health, avoidable health inequalities, arise because of the circumstances in which people grow, live, work, and age, and the systems put in place to deal with illness. The conditions in which people live and die are, in turn, shaped by political, social, and economic forces” (Nettleton et al, 2007). According to 2014-15 survey on indigenous smoking rates found that 42% of the indigenous Australians reported being the current smokers. It was found that they are 2.7 times higher in the prevalence of smoking compared to the non-indigenous. The proportion of population aged 15 years and over reporting they are a current smoker, by Indigenous status and age, 2014–15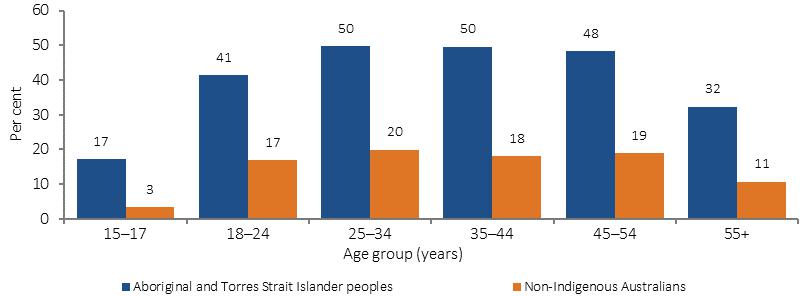 Source: ABS and AIHW analysis of 2014–15 NATSISS, 2014–15 NHS The higher smoking rate for indigenous Australian is associated with socio-economic factors in the most disadvantaged circumstances (Thomas, DP et al, 2008). Further studies have found that there is a higher density of tobacco outlets in more disadvantaged districts which also record a higher number of smokers (Marashi-Pour et al, 2015) Socio-economic factors such as education and unemployment have been considered to be the determinants of the smoking prevalence between indigenous and non-indigenous Australian. Their overlap may either grow or diminish prevalences along the social gradient (Marmot, 2015). (Hahn, R.A., Truman, B.I. 2015), those who have gone to school for more than 12 years are found to be less prevalent in smoking. It was also found that those living in low-income household show higher rates of smoking than high-income earners.
|
Question 2 Health issue代写Provide one example of a Primary Health Care intervention that is addressing this health issue for Indigenous Australians. Explain the impact this intervention is having on reducing inequity.
|
Training healthcare professionals in smoking cessation interventionsTraining of medical physicians may increase cessation of smoking rates to patients. This training will also increase the number of smokers to undergo advice on how to quit smoking. This is because training will increase the physician’s confidence, knowledge, skills and how to practice the smoking-related interventions. The training also encourages referral by the health service provider to the specialist smoking cessation services. The students who undergo the curricula retain the skills learned and they become more active in making smoking interventions. Although the tobacco curricula in medical schools vary the general objective of the training is similar.  The major reason why some doctors may not be active in tobacco use treatments is due to the lack of relevant training in medical schools. However, schools have incorporated the curricula in their training. Quit Victoria developed a systematic, comprehensive and tailored program for use in cessation training of medical professional in Australia. Impact of the intervention Health issue代写Due to the training of medical professionals on smoking cessation and other interventions smoking in indigenous Australian has significantly reduced. The intervention has encouraged referrals of smoking patients to the specialist in smoking cessation. Referrals increase the numbers of patients being helped to quit smoking which in return increases the number of Indigenous smokers in Australia. It has also helped doctor’s confidence in helping the patients because they have the required knowledge and skills to help their patient.
Training of medical professionals has increased the numbers of patients seeking smoking cessation over the few years. Patients also have confidence t the help they seek from these physicians. When a high number of indigenous Australian quit smoking, their health will improve and their economic status will also change because there will be no wastage of money to buy tobacco. Smoking cause health problems, therefore smoking cessation improve the health of the patient. The health burden to the government will be reduced as a result. |
Question 3 Health issue代写Discuss how cultural knowledge and sensitivity in health care may affect access Primary Health Care services. Provide one example based on your chosen health issue. |
|
Primary health care services not only require strong health system but also cultural support. the cultural barriers exist in the provision of medical cessation services in the indigenous Australian varying from the medical procedures and practices, language differences, and gender issues. These barrier result to miscommunications between the medical professional and the patient during cessation therapy programs to the indigenous Australian. Their poor outcomes are likely to emerge in cessation programs in areas exhibiting those cultural barriers. These barriers also lead to inequality in health care among the indigenous Australian. The studies have established that cultural knowledge and sensitivity may affect the willingness of indigenous people to use the mainstream health care centers.
Cultural identity has also affected how people perceive and seek health care. Health issue代写This refers to how people feel identified to a certain group in the society. Culturally, they tend to trust those people who hold the same beliefs, practice the same religion, are from the same country and social class, share ethnicity and have similar physiological characters. It has been proved difficult to deal with a person who holds such beliefs and there offering health care services become unsuccessful. Therefore it has come to be understood why indigenous people fail to seek medical assistance in various circumstances.
It has also been established that the health care system medical cover in Australia only manage to serve 40% of the population regardless of Australia having highly regarded health care system and the government-supported community services in the world. There is also a high number of health care centers in the metropolitan areas than rural areas, and also a high number of medical practitioners. The studies have found that health care system does not provide equal quality of healthcare to indigenous people compared to non-indigenous. Tobacco use among children from culturally diverse environments Health issue代写The studies have shown that the young people living in families where English is spoken are more likely to smoke than those living in families where there is the use of other languages. The studies show that young people who speak a language other than English at home shown a lower prevalence of tobacco use than those with a background of English speaking family. The logic behind this was how the environmental influences and cultural sensitivity has impacted on the prevalences to this risk behavior. The lower tobacco use by children from those families is because of the cultural attitude opposing tobacco use among children. These children are also likely to socialize with children speaking the same language, therefore, reducing peer influence (Larkins, et al 2016).
|
References

Marashi-Pour, S., Cretikos, M., Lyons, C., Rose, N., Jalaluddin, B & Smith, J. (2015). The association between the density of retail tobacco outlets, individual smoking status, neighborhood socioeconomic status and school locations in New South Wales, Australia, Spatial and Spatio-temporal Epidemiology, vol. 12, pp. 1-7.
Thomas, DP, Briggs, V, Anderson, IP & Cunningham, J 2008. The social determinants of being an Indigenous non-smoker, Australian & New Zealand Journal of Public Health, vol. 32, no. 2, pp. 110-116.
Marmot, M 2015. The Health Gap: The Challenge of an Unequal World, Bloomsbury Publishing: Great Britain.
S.Larkins, C.E. Woods, V. Matthews (2016) Responses of Aboriginal and Torres Strait Islander primary health-care services to continuous quality improvement initiativesFront Public Health, 3 (2016), p. 288
Hahn, R.A., Truman, B.I. (2015) Education improves public health and promotes health equity Int J Health Serv, 45 (2015), pp. 657-678
更多其他:艾莎代写 Case study代写 商科论文代写 研究论文代写 Review代写 Essay代写 艺术论文代写 人文社科代写 文学论文代写 心理学论文代写 哲学论文代写 cs论文代写 学术代写 Report代写 cs代写 代写论文


